Biotech Revolution: 2 Major Breakthroughs Reshaping US Healthcare by 2028

The landscape of US healthcare is on the cusp of an unprecedented transformation, driven by rapid advancements in biotechnology. We are not merely witnessing incremental improvements; rather, we are at the precipice of a genuine biotech revolution. By 2028, two particular biotech healthcare breakthroughs are set to fundamentally alter how diseases are diagnosed, treated, and even prevented, bringing with them profound implications for patients, providers, and the entire financial ecosystem of healthcare. This article delves deep into these pivotal innovations, offering insider knowledge and a comprehensive analysis of their potential financial impact.
For decades, medical progress often felt like a slow, arduous climb. Today, however, the pace of discovery has accelerated exponentially, largely fueled by our enhanced understanding of genomics, molecular biology, and artificial intelligence. The convergence of these fields is creating a fertile ground for innovations that were once confined to the pages of science fiction. Understanding these biotech healthcare breakthroughs is not just for scientists or investors; it’s crucial for anyone navigating the future of health and wellness in the United States.
The journey from a scientific concept to a widely adopted medical practice is complex, involving rigorous research, clinical trials, regulatory approvals, and significant financial investment. Yet, the potential rewards – both in terms of human health and economic returns – are immense. As we unpack these two major breakthroughs, we’ll explore not only the ‘what’ but also the ‘how’ and the ‘why’ of their projected impact on US healthcare by 2028.
The Biotech Revolution: 2 Major Breakthroughs Impacting US Healthcare by 2028
Breakthrough 1: Precision Gene Editing with CRISPR-Cas9 and Beyond
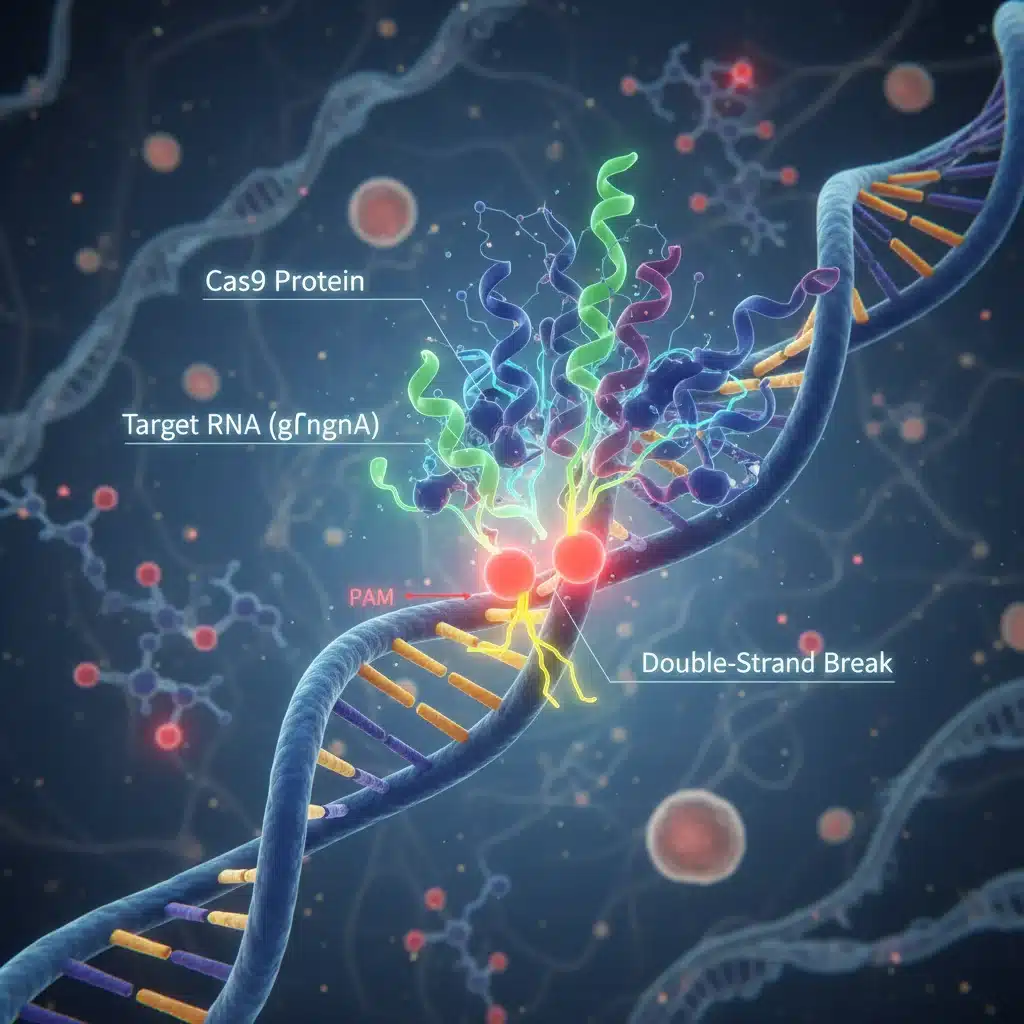
The first major biotech healthcare breakthrough poised to redefine US healthcare by 2028 is the advanced application of precision gene editing technologies, most notably CRISPR-Cas9. While CRISPR has been around for some time, its refinement, expanded therapeutic scope, and progress in delivery mechanisms are pushing it from experimental stages to mainstream clinical reality. This technology allows scientists to precisely cut and paste DNA sequences, offering an unprecedented ability to correct genetic mutations responsible for a vast array of diseases.
Insider Knowledge: The Evolution of Gene Editing
Initially, CRISPR’s potential was recognized for single-gene disorders like cystic fibrosis, sickle cell anemia, and Huntington’s disease. However, insider reports suggest that research is rapidly expanding into more complex conditions. New iterations of gene editing, such as ‘base editing’ and ‘prime editing,’ offer even greater precision and fewer off-target effects, significantly broadening the range of correctable mutations. These advanced techniques are akin to finding and fixing a single misspelled letter in a vast genetic library, rather than just deleting or inserting entire paragraphs.
Furthermore, the development of safe and efficient in vivo (within the body) delivery systems is a critical hurdle being rapidly overcome. Viral vectors, particularly adeno-associated viruses (AAVs), are proving effective in delivering the gene-editing machinery directly to target cells. Non-viral delivery methods, such as lipid nanoparticles, are also showing promise, potentially reducing immunogenicity and expanding accessibility. This progress means that instead of extracting cells, editing them, and reintroducing them (an expensive and complex process), gene therapy could become a one-time injection, making it far more scalable and accessible.
Clinical trials are already yielding remarkable results. For instance, therapies for certain forms of inherited blindness and severe combined immunodeficiency (SCID) are showing durable cures. By 2028, we anticipate FDA approvals for multiple gene-editing therapies targeting a wider spectrum of genetic disorders, moving beyond rare diseases to potentially address more common conditions with a genetic component.
Financial Impact: A Paradigm Shift in Healthcare Economics
The financial implications of precision gene editing are monumental. On one hand, these therapies represent a significant upfront cost. A single course of gene therapy can currently cost hundreds of thousands, if not millions, of dollars. This raises serious questions about accessibility, insurance coverage, and healthcare equity. Payers – both private insurers and government programs like Medicare/Medicaid – are grappling with how to integrate these ‘one-and-done’ curative treatments into their existing payment models, which are largely designed for chronic disease management.
However, the long-term financial picture is more nuanced and potentially transformative. For patients with chronic genetic conditions, the lifetime cost of managing their illness – including medications, hospitalizations, surgeries, and loss of productivity – can easily exceed the cost of a single gene-editing therapy that offers a permanent cure. For example, a child born with severe sickle cell disease might incur millions of dollars in healthcare costs over their lifetime. A curative gene therapy, even at a high price point, could be cost-effective in the long run.
By 2028, we expect to see innovative payment models emerging, such as outcomes-based agreements where payments are tied to the therapy’s long-term efficacy, or annuity models where the cost is spread over several years. The market for gene editing is projected to grow significantly, attracting substantial investment and fostering a new segment of the biotech industry. Pharmaceutical companies are aggressively acquiring or partnering with gene therapy startups, signaling their confidence in the future profitability and medical necessity of these biotech healthcare breakthroughs.
Furthermore, the ability to prevent or cure diseases could lead to a healthier, more productive workforce, reducing overall societal healthcare burdens. While the initial sticker shock for these therapies will be considerable, the potential for long-term savings and improved quality of life makes gene editing one of the most compelling biotech healthcare breakthroughs of our time.
Breakthrough 2: AI-Driven Drug Discovery and Personalized Medicine
The second transformative biotech healthcare breakthrough by 2028 is the widespread integration of Artificial Intelligence (AI) and Machine Learning (ML) into drug discovery, development, and the delivery of highly personalized medicine. AI is no longer just a tool for data analysis; it’s becoming an indispensable partner in every stage of the pharmaceutical pipeline and clinical decision-making, accelerating innovation and tailoring treatments to individual patient profiles.
Insider Knowledge: AI’s Role in Accelerating Innovation
Traditionally, drug discovery is a long, expensive, and high-risk endeavor, with a success rate of less than 10% from preclinical to approval. AI is fundamentally changing this equation. Insider information suggests that pharmaceutical companies are heavily investing in AI platforms that can analyze vast datasets of biological information – genomics, proteomics, imaging, and patient health records – to identify novel drug targets with unprecedented speed and accuracy. AI algorithms can predict how molecules will interact with biological targets, design new compounds, and even optimize existing drug candidates for efficacy and safety.
Beyond discovery, AI is revolutionizing preclinical and clinical trial phases. AI can predict which compounds are most likely to fail early, saving billions in wasted research. It can also optimize clinical trial design, identify suitable patient populations more efficiently, and monitor patient responses in real-time, leading to faster trial completion and higher success rates. For example, AI can analyze complex imaging data to detect subtle disease progression or response to treatment that might be missed by the human eye.
The true power of AI in medicine unfolds in personalized treatment. By analyzing an individual’s genetic makeup, lifestyle, environmental factors, and real-time health data (from wearables, for instance), AI can recommend the most effective drug, dosage, and treatment plan. This moves healthcare from a ‘one-size-fits-all’ approach to highly individualized care, minimizing adverse effects and maximizing therapeutic outcomes. Oncologists are already using AI to match cancer patients with specific therapies based on their tumor’s genetic profile, and this application is set to expand dramatically across other disease areas.
Financial Impact: Efficiency, Cost Reduction, and New Revenue Streams
The financial impact of AI-driven drug discovery and personalized medicine is multi-faceted. Firstly, it promises significant cost reductions in pharmaceutical R&D. By drastically shortening the drug development cycle and improving success rates, AI can save pharmaceutical companies billions of dollars. These savings can then be reinvested into further innovation or, ideally, lead to more affordable drug prices over time. The ability to bring effective drugs to market faster also means quicker returns on investment for biotech and pharma companies.
Secondly, personalized medicine, while initially seeming more complex, can lead to substantial long-term savings. By ensuring patients receive the right treatment at the right time, AI minimizes the costs associated with ineffective therapies, adverse drug reactions, and prolonged hospital stays. For instance, avoiding a costly chemotherapy regimen that is unlikely to work for a specific patient, and instead prescribing a targeted therapy that is highly effective, represents a massive saving for both the patient and the healthcare system. This precision approach reduces waste in the system.
Furthermore, AI will create entirely new revenue streams and business models. Companies specializing in AI-powered diagnostic tools, predictive analytics platforms, and personalized health management systems will flourish. Data-driven insights will become a valuable commodity, leading to collaborations between tech giants and traditional healthcare providers. Insurance companies may also leverage AI to better assess risk, manage chronic conditions, and incentivize healthy behaviors, potentially leading to more dynamic and personalized insurance plans.
By 2028, AI’s pervasive influence will not only make healthcare more efficient and effective but also reshape the economic incentives and competitive landscape of the entire biotech and pharmaceutical sectors. The integration of AI in these biotech healthcare breakthroughs is not just an enhancement; it’s a fundamental restructuring of how we approach health.

Synergies and Challenges: The Interconnected Future
These two biotech healthcare breakthroughs – advanced gene editing and AI-driven medicine – are not developing in isolation. In fact, their synergistic relationship will amplify their individual impacts. AI can accelerate the discovery of new gene targets for CRISPR, optimize guide RNA design, and even predict the outcomes of gene editing interventions. Conversely, gene-editing therapies will generate vast amounts of genomic and clinical data, which AI can then analyze to refine personalization strategies and improve diagnostic accuracy. This creates a powerful feedback loop, driving continuous innovation.
Navigating the Ethical and Regulatory Landscape
However, such transformative power comes with significant ethical and regulatory challenges. Gene editing raises profound questions about germline editing (editing genes in embryos or reproductive cells), which could lead to heritable changes. Societal discussions around ‘designer babies’ and equitable access to these powerful tools are paramount. Regulatory bodies like the FDA are working to establish clear guidelines that balance innovation with safety and ethical considerations, a process that will continue to evolve rapidly towards 2028.
Similarly, AI in healthcare brings concerns about data privacy, algorithmic bias, and accountability. Who is responsible if an AI makes a diagnostic error? How do we ensure that AI algorithms are not perpetuating existing healthcare disparities? Robust regulatory frameworks, explainable AI models, and transparent data governance will be crucial for the successful and ethical deployment of AI across US healthcare.
Infrastructure and Workforce Readiness
Beyond ethics, practical challenges remain. The US healthcare system will need significant infrastructure upgrades to fully leverage these biotech healthcare breakthroughs. This includes advanced bioinformatics capabilities, secure data storage, and specialized facilities for delivering complex therapies. Furthermore, the healthcare workforce will require substantial retraining. Physicians, nurses, and other allied health professionals will need to understand genomic medicine, interpret AI-generated insights, and counsel patients on highly personalized treatment options. Educational institutions and professional organizations are already beginning to integrate these topics into their curricula, but the scale of the necessary transformation is immense.
The Road Ahead: 2028 and Beyond
By 2028, the impact of these biotech healthcare breakthroughs will be undeniable. We will see a significant shift towards preventative and personalized medicine. Genetic screening will become more routine, identifying predispositions to diseases long before symptoms appear. This proactive approach, powered by AI and actionable through gene editing, will transform how individuals manage their health throughout their lives. Chronic diseases that once required lifelong management may become curable, and previously untreatable conditions will find effective interventions.
The financial implications will continue to evolve. While initial costs for some therapies will remain high, increased competition, economies of scale, and innovative payment models are expected to make these treatments more accessible. The focus will shift from managing illness to investing in wellness and long-term health outcomes, potentially leading to a healthier population and a more sustainable healthcare system in the long run.
However, achieving this utopian vision requires concerted effort from all stakeholders: scientists, policymakers, healthcare providers, industry leaders, and the public. Open dialogue, responsible innovation, and equitable access will be critical for harnessing the full potential of this biotech revolution. The future of US healthcare, shaped by these two major biotech healthcare breakthroughs, promises a healthier, more personalized, and ultimately more hopeful outlook for millions.
Conclusion
The biotech revolution is not a distant dream; it is happening now, and by 2028, its most profound impacts will be felt across the US healthcare system. Precision gene editing, particularly with advanced CRISPR technologies, offers the promise of curing genetic diseases at their root, fundamentally changing the trajectory of countless lives. Concurrently, AI-driven drug discovery and personalized medicine are accelerating the development of new treatments and tailoring existing ones to individual patient needs with unprecedented accuracy and efficiency. These biotech healthcare breakthroughs represent more than just scientific achievements; they are economic disruptors, ethical quandaries, and beacons of hope.
The financial landscape will be reshaped, moving towards value-based care where curative therapies, despite high upfront costs, prove cost-effective over a lifetime. New industries will emerge, and existing ones will adapt. While challenges related to ethics, regulation, and infrastructure are significant, the momentum behind these innovations is too powerful to ignore. As we approach 2028, these two biotech healthcare breakthroughs will not just be headlines; they will be the foundation of a healthier, more advanced, and profoundly transformed US healthcare system, offering a glimpse into a future where disease is not just managed, but often overcome.



